Africa CDC staff
In 2022, 61-year-old Mr Mebrhatu Gebreegziabher received his first dose of the COVID-19 vaccine during the pandemic, and as a pensioner residing in the remote, hard-to-reach area of Agebe village, Tanqa Milash woreda, Tigray Region in the northern part of Ethiopia, he looked forward to receiving a second dose to further protect himself.
“I had been looking forward to receiving my vaccination again against COVID-19 and other diseases,” he said.
For about three years, he could not receive these life-saving vaccines because of the prolonged conflicts in parts of northern Ethiopia, including the Tigray Region, which had largely disrupted healthcare service delivery.
Fortunately for Mebrhatu, through the community mobilisers engaged under the SLL programme, he heard about the integrated outreach for Non-Communicable Diseases (NCD) screening and COVID-19 vaccination organised by the Ministry of Health and Amref Health Africa.
He seized the opportunity under the SLL project, which Mastercard Foundation supported through Africa CDC.
He was also set to be screened for hypertension and diabetes mellitus. He hadn’t had these check-ups in years, since retiring from military service after 25 years. Back then, he had regular check-ups.
The outreach team screened Mebrhatu for hypertension and diabetes mellitus while administering the COVID-19 vaccine.
“I am going to champion awareness about the benefits of NCD screening and COVID-19 vaccination in my community to ensure my people live healthily and long,” he said.
Mebrhatu also committed to continuing regular Non-communicable Diseases (NCD) screening every three months as part of his healthy living and ageing journey.
Since the start of Phase II implementation of the SLL programme in the four regions of Afar, Amhara, Oromia and Tigray in Ethiopia, impactful stories of the underserved priority groups being reached, similar to that of Mebrhatu, abound.
Phase II of the SLL programme focuses on ‘geo-mapping and protection of healthcare workers and other high-priority groups such as the elderly and people living with chronic conditions through a life-course approach.’
Eliminating zero doses
In Ethiopia, health officials classify an estimated 3.9 million children as ‘zero-dose’, meaning these children have not received even a single routine vaccine. This critical public health challenge stems from a range of barriers, including ongoing conflicts, geographical isolation, and limited access to healthcare services.
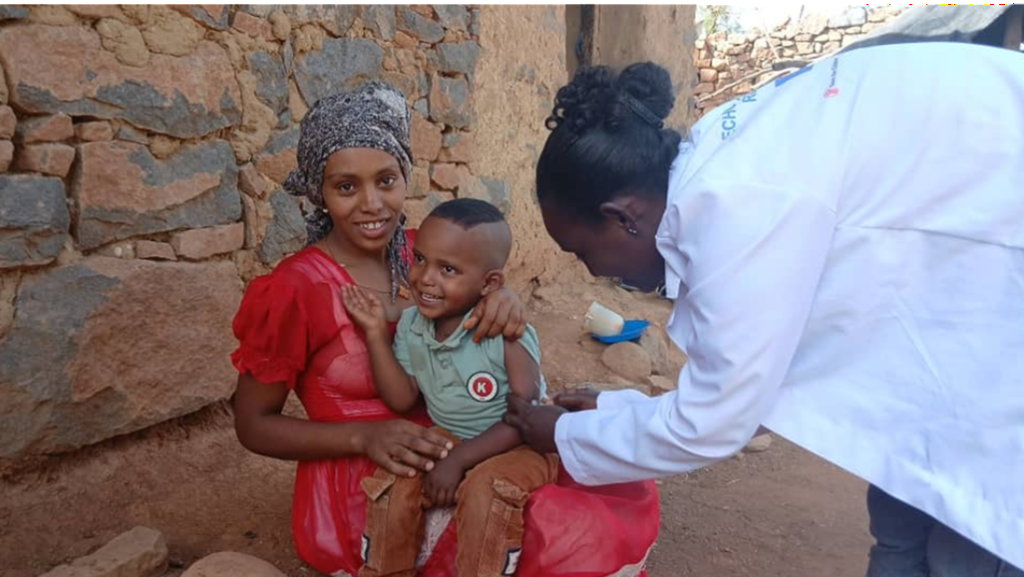
The Tigray region has been particularly hard hit. Years of conflict severely disrupted routine immunisation services, leaving thousands of children like Philmon Haylome, a 3-year-old boy from a rural village in Hayayle district, vulnerable to life-threatening, yet preventable diseases.
Philmon’s mother, Kisanet Teklay, recalls the uncertainty and fear during those years. “My child was born during the conflict and missed his vaccinations because services had stopped,” she said. “I believed that once a child got older, health workers wouldn’t vaccinate him anymore.” For years, Philmon remained at risk, unprotected against killing diseases like polio, measles, and pneumonia.
That changed with the arrival of the Saving Lives and Livelihoods Project, implemented by Amref Health Africa in partnership with the Africa CDC and funded by the Mastercard Foundation. As part of an integrated digital headcount and mobile vaccination campaign, SLL deployed health teams to reach underserved and remote areas, including Philmon’s village and home.
Through this targeted intervention, Philmon was finally reached and vaccinated, receiving three life-saving doses that protect him against seven deadly, vaccine-preventable diseases.
“Today, my child is vaccinated. I’m so happy. I no longer worry about him getting sick or spending money on treatment,” his mother says with relief.
The SLL Project continues to make significant strides in narrowing the immunity gap of the population. Innovative strategies like integrated digital headcounts and mobile outreach are helping health workers identify and vaccinate children in the most remote corners of Ethiopia. Philmon is just one of over 3,000 zero-dose children identified and immunised through this initiative in hard-to-reach areas.
Philmon’s journey is a shining testament to the impact of community-centred, equity-driven health interventions. Today, Philmon’s mother dreams of seeing her son grow up to become a medical doctor. This story shows how the project turns a tale of conflict and lost chances into one of safety, hope, and healthier futures, where childhood dreams can flourish.
In a recent project-supported campaign alone, over 40,000 children, including zero-dose and under-vaccinated children, received routine immunisations across four operational regions. This is part of SLL’s commitment to deliver over two million child and adult vaccine doses, contributing meaningfully to reducing the number of unimmunised individuals in Ethiopia.
Bringing health services to the people
Abdu Mohammed, a 49-year-old family man, lives in Gerseli Got 02 Kebele, a remote Mille district of Ethiopia’s Afar region. Like many in his village, Abdu faces significant challenges in accessing basic health services, especially life-saving vaccines for his family. Living in a hard-to-reach area puts his household at increased risk of preventable diseases, underscoring the urgent need for improved healthcare access in underserved regions.
“When we need to visit a health facility, our only option is to hire a Bajaj (three-wheeled taxi), which costs about ETB 350 for a one-way trip,” Abdu explained. “That’s simply unaffordable for us. The journey itself is difficult: rocky roads, scorching heat, and long travel times. For families like mine, especially those with young children, the cost and hardship involved often force us to delay or skip essential services like immunizations.”
The Afar people, who are one of the resilient communities, continue to face geographic and financial barriers that hinder their access to essential health services, particularly vaccinations. Fortunately for Abdu’s family, they were among the beneficiaries of the Integrated Headcount and Vaccination Campaign, supported by Amref Health Africa through the Saving Lives and Livelihoods (SLL) Project, funded by the Mastercard Foundation.
“Looking back, we used to live in fear because there were no nearby health services,” said Abdu. “I never imagined that healthcare would one day come directly to our home. Today, I’m truly grateful. My 4-year-old son, Mohammed Abdu, who had never received any vaccinations before, finally got the immunisations he needed. I also received the COVID-19 vaccine for the first time. Now, we no longer have to travel long distances or spend money we can’t afford. I deeply appreciate what this project has done for us.”
As part of the intervention, the SLL project deployed hundreds of mobile health teams who went door-to-door, reaching over 700,000 households. These teams identified missed and under-vaccinated individuals and provided COVID-19 and routine immunisations to more than 30,000 people on the same day, ensuring timely protection against vaccine-preventable diseases.
According to the WHO 2025 report, Ethiopia has an estimated 3.9 million “zero-dose” children, those who have never received a routine vaccine—and 54% of eligible adults remain unvaccinated against COVID-19. The SLL project is actively addressing this gap by reaching children and adults like Abdu and his son in remote, underserved areas.
Phase II of the SLL project is strategically designed to serve the most marginalised communities, including those in hard-to-reach, conflict-affected, and geographically isolated areas. With a bold commitment to equity and access, the project is ensuring that no one is left behind, bringing life-saving vaccines to everyone, everywhere.
The stories of Mebrhatu, Philmon, and Abdu echo the positive impact created by the SLL programme in reaching the priority groups, particularly the elderly in the hard-to-reach areas of Ethiopia who have remained underserved largely due to the prolonged conflicts that have disrupted routine healthcare delivery services in their communities.